The allergy test, which shows sensitization due to IgE, is an important test that helps diagnose suspected allergic conditions. Besides the advantages of allergy testing, there are also disadvantages. In allergy tests, expectation finds the cause of the allergic disease that occurs in our body. In this article, we wrote the allergy tests so that we could describe them with it’s pros and cons.
Allergy Test Methods
Allergy tests can be done from the skin or blood. Skin allergy test is called skin prick test.
What is the Skin Prick Test?
It is a test made from the skin and shows sensitization due to IgE. The skin prick test is a useful test due to its rapid results, simplicity and low cost. Skin prick tests and other skin test results show the sensitivity due to IgE, which we call type 1, and give us information about food, inhalent allergens, pet allergens, insect, mold and drug allergens. It is very important that these tests are interpreted by allergists who are capable of interpreting these tests. It is of great importance that children from birth to 18 are interpreted by pediatric allergists and those over 18 by adult allergists.
Basophil activation test
Basophil activation tests are molecular-based allergy tests and are used to better define patients’ IgE profiles.
Allergy Tests
Allergic diseases are one of the most common diseases worldwide and the burden of these diseases continues to increase. An accurate diagnosis, combined with appropriate treatment, requires the use of appropriate tests to confirm allergen sensitivity and detailed information about exposure to the assumed allergen. Skin tests, especially skin prick testing, represent the most reliable and cost-effective tool for the diagnosis and treatment of IgE-mediated diseases. With allergy tests, the allergic cause of nose, eye, skin, mouth and lung difficulties can be found.
Once the diagnosis has been made and the relevant allergens identified, specific treatments are required to achieve appropriate, long-term results, including medications, environmental control measures and / or allergen immunotherapy (AIT) called allergy vaccine therapy. Therefore, allergy testing is very important in allergy diagnosis.
How many types of allergy skin tests are there in the diagnosis of allergies?
1) Skin Prick Test (SPT): It is the first test used to diagnose type I, sudden, IgE-mediated allergy. Safe, has high sensitivity and good specificity when done and interpreted correctly; A specific variant of type I skin testing is the prick-prick test (PPT) with natural allergens.
2) Intradermal Test (IDT): This can be used to evaluate both immediate IgE mediated allergy and delayed type hypersensitivity by reading time. It is a test that can be effective in showing sensitivity compared to SPT.
3) Patch test: Used for delayed type, cell-mediated, hypersensitivity reactions. It has nothing to do with IgE mediated allergy. It is a method mostly used in the diagnosis of contact allergic diseases.
What are blood allergy tests?
Blood allergy tests are a test that can be useful in determining the cause of allergic diseases.
1)Total IgE Test: This test is a test that gives rough information about the allergic nature of the person. While a high result indicates that you are likely to have allergies, it does not necessarily indicate that you have allergies. Normal or miscarriage does not necessarily indicate that you are allergic, but it does indicate that you are less likely to have allergies.
2)Allergen-specific IgE tests: It is a test that shows IgE values against allergy-causing substances or their components. It can be considered as the form of the skin allergy test made from blood.
3)Basophil activation test: The basophil activation test, on the other hand, is a difficult test to perform and is a test performed in some special allergic diseases.
Skin allergy tests (Skin Prick Tests)
Charles H Blackley administered the first skin test in 1865. In 1924, Lewis and Grant first described the skin prick test method.
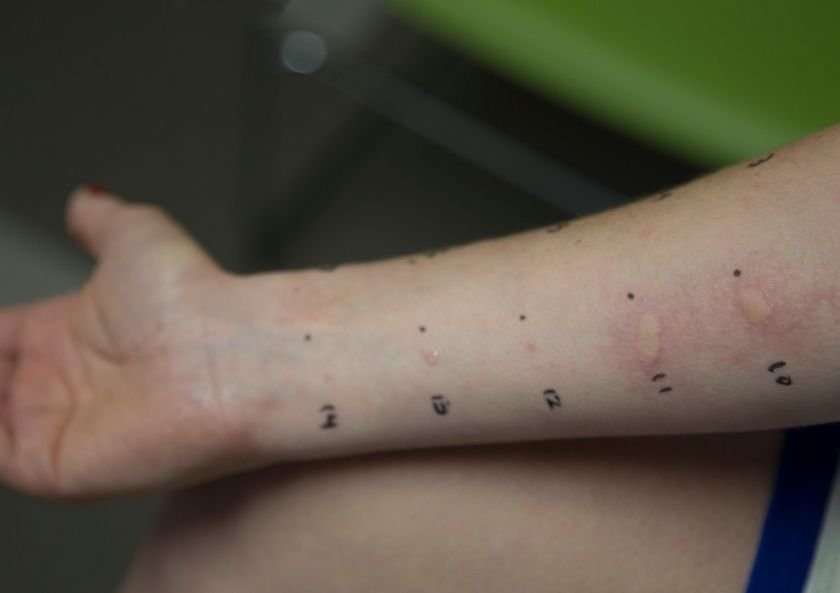
The skin prick test is the simplest method used to evaluate the presence of sensitivity due to IgE in humans. In the skin prick test, the substances in the mast cell cause swelling and redness on the skin by binding of the allergen-specific IgE bound to the mast cells in the skin after certain allergens contact with the skin of allergic individuals through a lancet. By evaluating this swelling and redness, the allergy test is interpreted. It is a small indicator that shows the presence of an allergic disease in our body.
When should skin prick tests be done?
To perform a skin prick test, medical history and examination are required first. If the history and examination findings suggest an allergic disease due to IgE, which we call type 1, this test can be done. Skin prick test is appropriate especially in cases of asthma, allergic rhinitis, eye allergy, food allergy, bee allergy, medications and occupational allergies due to inhalen allergens such as house dust mite, pollen, pet epithelium. As a result;
Conditions that may be appropriate to have a Skin Prick Test are:
-Asthma
-Allergic Rhinitis
– Eczema (Atopic dermatitis) (in those with suspected IgE-related allergies)
– Suspected food allergy (in cases where allergic shock is suspected, oral allergy syndrome, sudden hives, eczema due to food allergy)
-Suspected drug allergy
-Bee and insect allergies
-Suspected occupational allergic diseases
-In case of chronic hives suspected of a triggering allergen
-Skin prick test can be performed in rare cases such as eosinophilic esophagitis, eosinophilic gastroenteritis or allergic bronchopulmonary aspergillosis, suspected of allergy related to IgE.
If it is not appropriate to perform a skin prick test:
-In case of suspected food intolerance
-In the case of chronic hives without an allergen-triggered feature
-Those who want to have a test to lose weight
-Those with symptoms thought to be associated with food additives, preservatives, colorants
-Doing to evaluate the effectiveness of allergy vaccine.
-In situations with lung symptoms with irritants such as perfume, detergent odor and chemicals
-To screen for allergies without any symptoms
-In cases of skin rashes without allergic symptoms and migraine, allergy testing does not help. Testing may be considered if an allergic condition to hormones has developed.
-In case of prolonged fatigue
Skin prick tests give a reliable result in determining the cause of allergic disease. However, the clinical significance of the sensitivity detected in skin prick tests should be carefully considered. Because a positive result in an allergy test may not always be a cause of allergic disease. Accurate diagnosis is very important for determining the exact cause of allergy, taking correct avoidance measures, and choosing the right allergens when necessary, when choosing an allergy vaccine.
The importance of clinicians performing and interpreting skin prick tests
A clinician with sufficient knowledge of the important, relevant allergens based on the patient’s history and geographic location should decide which specific allergens are tested and interpret the test results with the clinic. Skin prick tests should be performed in clinics with the knowledge and experience that can perform emergency treatment in case of severe allergic reaction or allergic shock. When standardized allergy tests are used in clinically stable patients, the risk of developing serious reactions such as allergic shock is extremely low.
How Should the Allergy Test Result Be?
Like any medical procedure, allergy tests should be recorded and given to patients as a test result.
In the allergy test result document, the patient’s name and surname, date of birth, date of the allergy test, the name of the doctor who performed the test, the phone number, the region tested, the name of the technician / nurse / doctor / healthcare intern who performed the test, the type of device used, and the relevant results are negative. The positive control results should be the name of the tested allergens, the Latin name and the name of the allergen manufacturer, the dilution rate if the allergen extract is diluted, the extent of swelling and redness for each allergen, the post-test reading time (usually 15-20 minutes). In addition, it is important to optionally check the check box in the consent form that informs that they do not use drugs that may affect the result before starting the test. The allergen extract source, lot number and expiry dates can be kept separately.
What are the medications that can affect allergy tests:
Before the allergy test, consent should be obtained that drugs that may affect the test are not taken. According to the recommendations of the American Academy of Allergy, Asthma and Immunology, the American College of Allergy, Asthma and Immunology, and the European Academy of Allergy and Immunology, the list of drugs that should be discontinued before the allergy test and how long before is reported in the table below.
Table 1: Recommendations regarding drugs that may affect skin prick tests
| • Stop H1-antihistamines for the required number of days before performing skin tests, according to the properties of the drugs listed below (most antihistamines 4-5 days, ideally 7 days). |
| • Stop H2-antihistamines 24 hours before doing skin tests. |
| • Stop anti-depressants with H1-antihistamine activity 1 week before the test (consult the prescription if possible). |
| • It is not necessary to stop leukotriene antagonists. |
Table 2: Drugs affecting allergy testing and withdrawal times
| Medicines | Generic drug | How many days before the test should be stopped |
| H1-antihistamines | ||
| First generation | chlorpheniramine | 2-6 |
| clemastine | 5-10 | |
| cyproheptadine | 9-11 | |
| dexchlorpheniramine | 4 | |
| diphenhydramine | 2-5 | |
| Hydroxyzine | 5-8 | |
| promethazine | 3-5 | |
| tripelennamine | 3-7 | |
| Second generation | Azelastine nasal | 3-10 |
| ebastine | 3-10 | |
| cetirizine | 3-10 | |
| fexofenadine | 2 | |
| loratadine | 7-10 | |
| Desloratadine | 3-10 | |
| levocetirizine | 3-10 | |
| Bilastine | 4-5 | |
| Levocabastin nasal | Do not suppress skin tests | |
| Levocabastine ophthalmic | Do not suppress skin tests | |
| rupatadin | 3-7 | |
| Tricyclic antidepressants and tranquilizers | desipramine | 2 |
| Imipramine | >10 | |
| doxepin | 6-11 | |
| Doxepin topical | 11 | |
| H2-antagonists | ranitidine | 1 |
| Anti-IgE monoclonal antibody | omalizumab | Prick tests can be done after 6 weeks, but false negative results may occur for up to a year. |
| Cysteinyl leukotriene receptor antagonists | Montelukast | Does not suppress skin tests |
| zafirlukast | Does not suppress skin tests | |
| Short-term oral corticosteroids | 30mg prednisone daily for 1 week | Does not suppress skin tests |
| Prolonged and relatively high doses of corticosteroids | > 20 mg / day | Possibility of suppression of allergy test reactions |
| Strong topical corticosteroids | > 3 weeks | Suppresses allergy test results in areas where they are applied |
| Local anesthesia | EMLA (Eutectic Blend of Local Anesthetics) cream | 1 hour before test suppression (only suppresses erythema) |
Allergy solutions used in allergy tests
The solutions to be used in allergy tests vary according to the type of allergy disease and the place where they live. Allergy test solutions used for allergy tests consist of a mixture of allergenic (proteins, glycoproteins, polysaccharides) and non-allergenic components (lipids, salts, pigments, metabolites) obtained from the allergen source. Therefore, crude extracts consist of original sensitizers and cross-reacting proteins. Generally, allergens are mainly proteins or glycoproteins, but carbohydrates or other low molecular weight chemicals can cause allergic sensitization when converted into complete antigens.
Allergen extracts are usually obtained from natural sources through aqueous extraction. Their composition and biological properties can be affected by the quality and purity of the source material, extraction and processing methods, and storage conditions. Extras should not contain more than one allergenic source (mixtures can be used if they contain sources from a homogeneous taxonomic family) and should not contain interacting preservatives such as thiomersal.
Recombinant Allergy Test Solutions
Diagnostic extracts made from recombinant or highly purified allergenic proteins are available as approved in some countries for allergy diagnosis. Recombinant and natural allergen preparations were evaluated and compared. In general, skin testing with synthesized allergens is highly specific and prevents false positives from occurring by eliminating cross-reactive allergens. However, the precise role of recombinant allergens as an in vivo diagnostic tool continues to be fully determined.
Standardizing Allergy Test Solutions
Allergen extracts used for diagnosis should ideally be standardized. Standardization facilitates the comparison of extracts from different manufacturers, batch-to-batch variability, and the reliability and reproducibility of test results.
Current standardization is particularly important in European countries where strict regulatory rules sometimes cause problematic and costly registration of some products.
Allergic extracts should also be cost effective.
Stability and strength of allergen test extras are also important issues. Allergen skin test solutions are generally preserved with 50% glycerin, as the allergen extract potency degrades over time, accelerated by dilution and higher temperatures. All extracts should be stored in a refrigeration unit at 2–8 ° C to increase stability. For diagnostic use, both standardized and non-standardized products are commercially available with labeling in various power units
Table 3: Examples of skin test concentrations of standard and non-standard allergens
| Allergen product | Skin prick test concentration | Intradermal test concentration |
| Standard short ragweed | 1:20 w/v | 1:1000 w/v |
| Standardized cat epithelium | 10.000 BAU/mL | 200 BAU/mL |
| Standardized grass pollen | 10.000-100.000 BAU/mL | 200 BAU/mL |
| Standard Hymenoptera venoms | 100 μg protein / mL | 0.1-1 μg protein / mL |
| Standard mites | 10.000 AU/mL | 200 AU/mL |
| Non-standard allergens | 1:40-1:20 w/v | 1:1000 w/v |
What should be the number of allergy tests?
According to the world-recognized allergy skin testing study, it has shown that for respiratory / conjunctival allergies, it is not necessary to include multiple allergen extracts for skin testing. The total number of allergens tested depends on the local exposure framework, as noted above. The recommended panel for respiratory allergy can contain 18 allergens:
-Alder (Alnus incana),
-Birch (Betula alba / verrucosa),
-Cypress (Cupressus sempervirens / arizonica),
-Nut tree (Corylus avellana),
-Sycamore tree (Platanus vulgaris),
-Grass mix (including Poa pratensis, Dactilis giomerata, Lolium perenne, Phleum pratense, Festuca pratensis, Helictotrichon pratense),
-Olive tree (Olea europea),
-Common wormwood (Artemisia vulgaris),
-Blackweed (Ambrosia artemisiifolia),
-Alternaria alternata (tenuis),
-Cladosporium herbarum,
-Aspergillus fumigatus,
-Wall basil,
-Cat (Felis domesticus),
-Dog (Canis familiaris)
-Dust mite (Dermatophagoides pteronyssinus / farinae) and
-Cockroach (Blatella germanica).
Testing with Blomia tropicalis is recommended in tropical countries.
When testing babies, the number of tests performed should be much less.
Information on cross-reactivity between allergens is important when interpreting the results. Cross-reactivity explains the phenomenon in which an immediate skin reaction with a particular allergen (original sensitization) can also be caused by other similar allergens and is explained by IgE cross-reactivity to homologous (cross-reactive) allergens. Cross-reactivity of pollen is common in the case of highly conserved proteins between taxonomically related plants or between different species.
| Cross reaction groups | Representative breeds | |
| Grass pollens | Pooideae | Poa (blue), Bromus (bromine), Dactylis (orchard), Festuca (fescue), Lolium (annual rye), Agrostis (redtop), Anthoxanthum (sweet spring), Avena (cultivated oats), Holcus (velvet), Phalaris (reed canary), Phleum (timothy), Agropyron (quack), Elymus (wild rye), Secal e (cultivated rye), Triticum (cultivated wheat) |
| Chloridoideae | Cynodon (Bermuda), Bouteloua (blue gray, mosquito Grass), Distichlis (salt) | |
| Panicoideae | Paspalum (Bahia), Sorghum (Johnson), Panicum (Pra grass), Zea (corn) | |
| Tree pollens | Aceraceae | Acer (Maple) |
| Betulaceae | Alnus (alder), Betula (tree), Corylus (nut) | |
| Cupressaceae | Cupressus (cypress), Juniperus (juniper and cedars), Taxodium (bald-cypress), Crypto currency (Japanese cedar) | |
| Legumes | Acacia (Mimosa), Robinia (Carob), Prosopis (Mesquite Tree) | |
| Fagaceae | Quercus (oak), Fagus (beech) | |
| Juglandaceae | Carya (hickory and pecan), Juglans (walnut) | |
| Moraceae | Morus (mulberry), Broussonetia (paper mulberry) | |
| Oleaceae | Olea (olive), Fraxinus (ash), Ligustrum (privet) | |
| Pinaceae | Pinus (pines) | |
| Platanaceae | Platanus (sycamore) | |
| Salicaceae | Populus (cottonwood and poplars), Salix (willows) | |
| Ulmaceae | Ulmus (elm) | |
| Weed pollens | Chenopodiaceae | Atriplex (scales and saltbush), Chenopodium(lamb’s quarter), Salsola (Russian thistle), Kochia(firebush), Allenrolfea (iodine bush) |
| Asteraceae: Artemisia | Artemisia (wormwood, sage) | |
| Asteraceae: Ambrosia | Ambrosia (ragweeds), Xanthium (cocklebur), Iva (poverty weed hemp) | |
| Amaranthaceae | Amaranthus (careless grass, pig weed), Acnida (Western water hemp) | |
| Plantaginaceae | Plantago (banana) | |
| Polygonaceae | Rumex (dock and sorrel) | |
| Nettles | Pariet |
A representative genus are members of the same botanical family or subfamily. Manufacturers currently offer allergen products derived from one or more species of each listed genus.
Generally, testing with fewer allergens to suspected allergens is required in infants and very young children (<2 years of age) because children are unlikely to be as allergen-sensitive as older children and adults. Allergic sensitization in young children would be more appropriate with allergens with intense and / or long-term exposure to allergens encountered early in life, especially food, house dust mites, indoor molds and animal hair instead of pollen.
Relatively few foods account for the majority of IgE-mediated allergic reactions in both children and adults.
The more common food allergens in infants and young children are: cow’s milk, chicken eggs, peanuts, tree nuts, soybeans and wheat, and adults peanuts, tree nuts, fish, crustaceans, mollusks, fruits and vegetables.
However, this generalization should not preclude the possibility of further testing if multiple or hidden food allergies are suspected. The allergy test called the Prick-Prick test, in which a fresh food sample is immersed, is tested with the food itself. This test may be more accurate in the diagnosis of food allergies than with allergy solutions.
Table 5 Suggestions for Skin Prick Tests
- Identify skin test allergens relevant to specific geographic area
- Whenever possible, standard allergen products should be used for skin testing.
- Clinical history should guide skin testing as there is potential for false positive responses.
- More allergens may need to be assessed in regions with greater biodiversity and warmer climates.
- Limit the number of allergens used in skin testing by considering cross-reactions and eliminating non-significant allergens in the area of exposure.
- Add positive (histamine) and negative (buffer) controls.